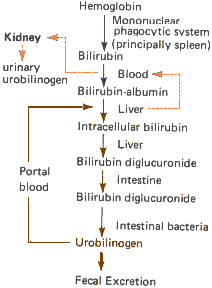
 Jaudice is the visibly evident symptom of amber coloration of the skin and sclera from increased circulating concentration of the pigment bilirubin, a heme degradation product. Senescent and/or damaged red cells are phagocytized in the reticuloendothelial system, where hemoglobin degradation results in the formation of bilirubin. Newly formed bilirubin is transported in the circulation tightly bound to albumin and is taken up by the liver, where it is conjugated with glucuronic acid and actively secreted into the bile canaliculi. A small portion of water soluble, conjugated bilirubin diffuses from hepatoctes into plasma. Being water soluble, conjugated bilirubin is not bound to albumin and is freely filtered by the glomeruli, in contrast to unconjugated bilirubin.
Jaudice is the visibly evident symptom of amber coloration of the skin and sclera from increased circulating concentration of the pigment bilirubin, a heme degradation product. Senescent and/or damaged red cells are phagocytized in the reticuloendothelial system, where hemoglobin degradation results in the formation of bilirubin. Newly formed bilirubin is transported in the circulation tightly bound to albumin and is taken up by the liver, where it is conjugated with glucuronic acid and actively secreted into the bile canaliculi. A small portion of water soluble, conjugated bilirubin diffuses from hepatoctes into plasma. Being water soluble, conjugated bilirubin is not bound to albumin and is freely filtered by the glomeruli, in contrast to unconjugated bilirubin.
| total bilirubin | < | 1.4 mg/dl |
| direct bilirubin | < | 0.4 mg/dl |
| urine bilirubin | undetectable | |
| urine urobilinogen | undetectable |
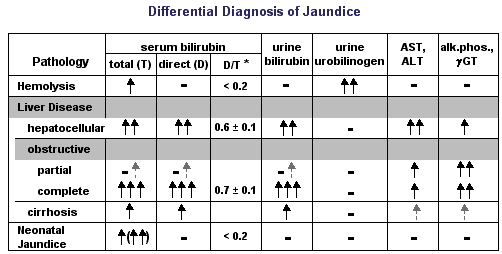
Pathophysiology of Jaundice
The circulating concentration of bilirubin may become elevated as a consequence of |
| *D/T is not typically reported, but is included here to emphasize that direct bilirubin is the predominant fraction in both hepatocellular and obstructive liver disease. |
Cirrhosis refers to chronic, advanced liver disease with replacement of hepatocytes with fibrous tissue and insiduous loss of function.
The enzyme, glucuronyl transferase is often deficient in neonates and unconjugated bilirubin accumulates, usually only to a mild degree. In extreme cases, the albumin binding capacity may be exceeded (~ 20 mg/dl) and unconjugated bilirubin deposits in fatty tissue, including the central nervous system. Kernicterus refers to staining of basal ganglia and other CNS structures and consequent permanent neural damage. Kernicterus is thought to be restricted to neonates because of the immature blood-brain barrier.